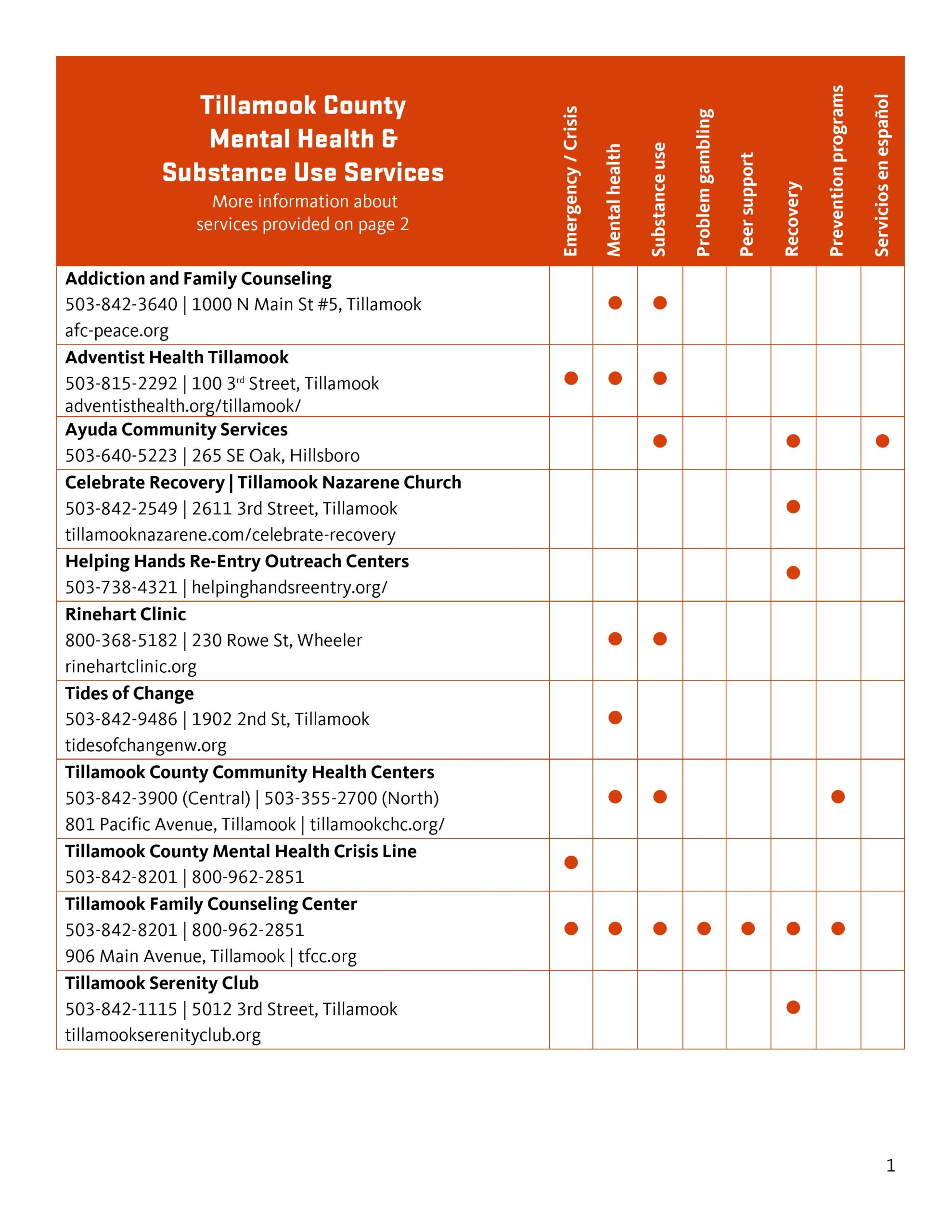
EDITOR’S NOTE: April is Sexual Assault Awareness Month, so Leanna Coy’s article about the connections between Intimate Partner Violence (IPV – IPV or Domestic Violence Awareness month is October) is timely. These topics need to be talked about every month to shine a light on the impacts of sexual assault, PTSD, trauma and more. If you or someone you know has experienced a sexual assault or domestic violence, please reach to our local support team at Tides of Change – www.tidesofchangenw.org
See additional story about events, proclamations and outreach for Sexual Assault Awareness Month.
By Leanna Coy, FNP-BC
Perimenopause is the time in life when hormone levels begin to fluctuate and decline. These changes trigger physical symptoms and can affect a person’s health. If someone has a history of domestic abuse, they may experience perimenopause differently. In fact, studies show a unique health crossroad between perimenopause and intimate partner violence.
What is Intimate Partner Violence
Intimate partner violence, or IPV, is a form of domestic abuse. IPV includes patterns of behavior in relationships used to gain or keep control. Abusive behaviors may be physical, sexual, or emotional. Stalking, aggression, and threats by a current or former partner are also IPV.
In Oregon, 42% of women report experiencing IPV at some point in their lives. Each person experiences IPV differently. The severity and frequency of abuse vary by circumstance. IPV is disruptive and harmful. It can lower quality of life, cause missed work, physical injuries, safety concerns, and police reports.
IPV is linked with many acute and chronic health issues.
- Cardiovascular: obesity, high cholesterol, high blood pressure.
- Digestive: irritable bowel syndrome, persistent indigestion or upper abdominal pain, chronic constipation and/or diarrhea.
- Reproductive: pain during sex, STDs and HIV, painful urination, unplanned pregnancy, chronic pelvic pain.
- Neurological: headaches, migraines, dizziness, memory problems, vision problems, hearing problems, difficulty concentrating, mood changes, dementia, and sleep problems.
- Endocrine: diabetes, menopause symptoms, night sweats, dyspareunia, vaginal dryness and irritation.
- Mental health: PTSD, anxiety, depression, self-harm, sleep disorders, substance abuse.
Perimenopausal Changes
Perimenopause typically begins in the mid-40s but can start as early as mid-30s or as late as mid-50s. During this phase of life, the ovaries begin producing less estrogen, resulting in hormonal fluctuations. The change in hormone levels triggers some common symptoms. Most people going through perimenopause will experience at least one of these symptoms:
- Changes to menstrual cycles, including missed or irregular periods, and bleeding that is lighter or heavier than usual
- Difficulty sleeping
- Night sweats
- Hot flashes
- Mood changes, such as anger, irritability, depression, and anxiety
- Low sex drive
- Vaginal dryness or discomfort during sex
- Urinary urgency
Overlapping Conditions and Symptoms
Menopause researchers are finding that symptoms appear to start earlier and are often worse for people with a history of IPV.
A four-year study of women ages 40 to 80 found more menopause symptoms in those with a history of abuse. These issues include sleep problems, hot flashes, night sweats, painful sex, and vaginal irritation. Another study found that people with a history of abuse report more frequent and severe vasomotor symptoms like hot flashes and night sweats.
Early perimenopause, which is symptoms starting before age 45, shows up often in those with a history of IPV. Researchers believe the early symptoms relate to stress regulation imbalances from the abuse. This is especially true if the violence happened early in life.
Some memory loss is a normal part of aging and may begin in perimenopause. Often this shows up as forgetting names or why you walked into a room. Traumatic brain injuries or strangulation from abuse may cause greater cognitive and neurological changes. These changes can include memory loss, mood swings, sleep problems, and headaches.
Depression is quite common for individuals with both a history of abuse and perimenopause. Perimenopause is often described as a “window of opportunity” for depression to start. This could be new or worsening depression due to the lower estrogen levels.
Despite earlier and more severe symptoms, people with a history of IPV don’t seek perimenopause care. Instead, many try to manage on their own. But treatment is available.
If you think you may have perimenopause symptoms, don’t wait. Take action now by scheduling an appointment with your healthcare provider. During your visit, make sure to openly discuss all your symptoms and concerns. This helps the provider to fully understand your needs and recommend the best treatment options. If you have a history of IPV, share this information with so your provider can address any additional needs.
Remember, seeking healthcare is a proactive way to improve your well-being during perimenopause and beyond. Take steps to address symptoms early by seeking medical care and support. Doing this is a powerful form of self-care that may help protect your health and quality of life as you age.