Enrique Garcia, a community health care worker in Keizer, wrote:
My first vaccine was the best experience; after the second shot got chills and little bit of headaches along with body temperature change, but all within the first 24 hours. I am Latino and always trying to lead by example. We have our Latino population around us here in Marion County, and they know who I am. I work in health care and would like to continue to assist patients, and that’s another reason I want to protect the people that I am in touch with by getting the vaccine.
Anna Tiwari, a doctor at Canyonville Health and Urgent Care, wrote:
We are a four-provider practice in rural Oregon. It was harder for us to get the vaccine as my staff is not affiliated with a hospital. There were a lot of misconceptions about the vaccine, so it was important to set an example. The first dose was a breeze, minor arm pain for 6 to 8 hours. It did encourage a couple more of our staff members to accept the vaccine when it was available to them. After the second dose, I had some body aches and sweats and a headache, nothing that a 250 mg of Tylenol couldn’t fix. Though people are concerned about the vaccine side effects, it makes you wonder how much worse the disease is likely to be, something I am not keen to experience. We treat an elderly population, and they need to be protected, and we need to be there for them and not be out sick. It’s just as important to reassure the patients that the vaccine is a lifesaving measure for not just you but for everyone around.

Rose Rockwood, an administrator at Country Side Living in Canby, wrote:
Country Side Living’s vaccine experience was well organized and seamless. Due to a personal fear of needles, I was very anxious about receiving the vaccine. The nurse was very empathetic of my fear and provided me with a detailed step-by-step process explanation. I was able to relax and receive my vac
cine successfully. I experienced no negative side effects following the vaccine. I have various reasons for feeling passionate about receiving the vaccination: The population I work with is of the highest risk for having complications due to COVID. Additionally, I have multiple family members (grandparents and children) who are at risk.
The what, where and why of COVID-19 data: Hospital capacity
OHA produces a variety of data related to Oregon’s COVID-19 response. Because keeping up with these data can be difficult, we’ll be highlighting some insights about OHA’s COVID-19 data and analyses in an occasional series. Today, we’ll focus on hospital capacity data.
OHA collects data from hospitals through Oregon’s Hospital Capacity Web System (HOSCAP). Each hospital reports daily numbers of patients with COVID-19 and the total and available staffed beds at their facility to OHA. “Staffed beds” are the number of beds a hospital has ready to support patient care, including staff and equipment. By subtracting available beds from total staffed beds, OHA can calculate how many hospital beds are currently in use. Hospitals also report other specific information to OHA, including staffed beds in certain hospital units (e.g., intensive care units) as well as the number of patients requiring mechanical ventilation.
It is important to note that staffing challenges can be fluid and can affect bed capacity in real-time. Such staffing limitations may not be captured in HOSCAP and may further limit bed capacity.
Hospital capacity data are helpful indicators used by hospitals, health systems and state health authorities for health planning during the pandemic. When the number of hospitalized COVID-19 patients rises, it is a warning that the demands on the health care system will also increase.
When hospital capacity becomes strained, hospitals can implement surge plans to conserve resources and capacity. These plans may involve canceling elective surgeries, moving ICU patients who no longer need intensive care services to other areas of the hospital, and even repurposing beds from other hospital units into ICU beds.
HOSCAP data are visualized as daily counts of current staffed hospital bed capacity and hospitalizations over time. Current HOSCAP data highlights can be found on Oregon’s COVID-19 Update dashboard (top), while more detailed information can be found on the Oregon COVID-19 Hospital Capacity dashboard (bottom).
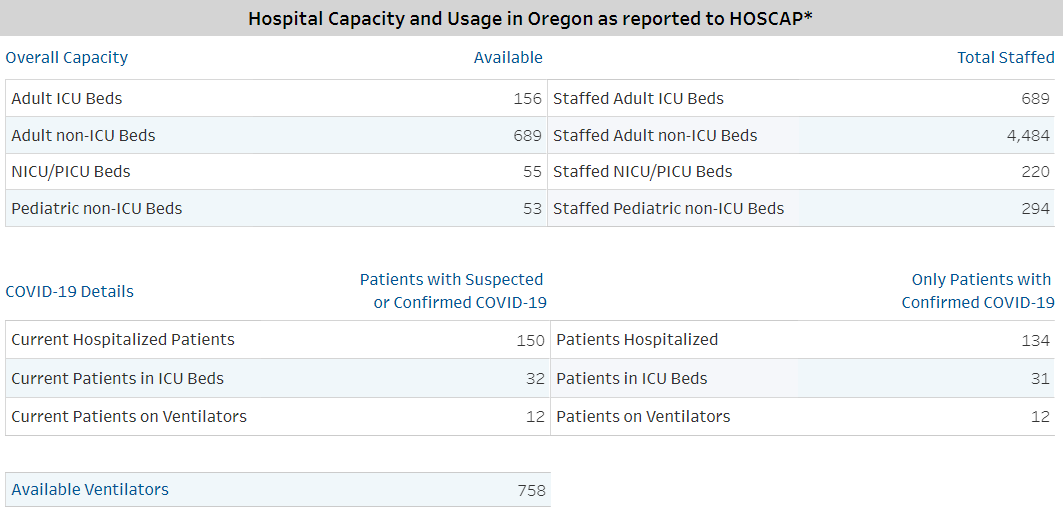

HOSCAP data on Oregon’s COVID-19 Update dashboard.
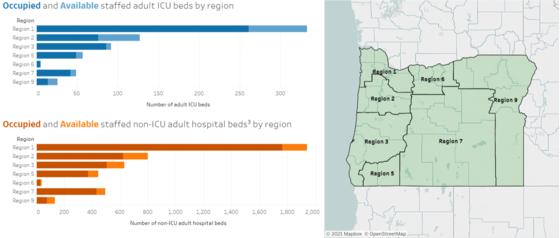
HOSCAP data on the Oregon COVID-19 Hospital Capacity dashboard.
OHA has reported that the number of hospitalized patients with COVID-19 across Oregon is 134, which is 15 fewer than one week ago. Of these patients, 31 are in intensive care unit (ICU) beds, which is two fewer than one week ago. While modest decreases, both numbers reveal a downward trend that is providing a momentary sigh of relief for health care professionals and patients across the state.
For more research and analysis on the COVID-19 situation in Oregon, check out our Weekly Data Report, our Weekly Outbreak Report or our Epidemic Trends and Projections report.
Updates to county risk levels to take effect March 12- Tillamook County to move to “Moderate” Risk
Today, county risk levels under the state’s public health framework to reduce transmission and protect Oregonians from COVID-19 have been updated. The framework uses four different risk levels for counties based on COVID-19 spread — Extreme, High, Moderate and Lower — and assigns health and safety measures for each level.
Beginning this week, counties may be given a caution period if they reduced their COVID-19 spread enough to move down in risk level in the previous two-week period but their numbers went back up in the most recent two-week period. The caution period will allow counties to refocus efforts on driving down creeping case numbers and give local businesses additional certainty on their plans for operating. If, at the end of the caution period, case rate data still puts the county at a higher risk level, the county will move to that level.
Effective March 12 through March 25, there will be two counties in the Extreme Risk level, nine at High Risk, 12 at Moderate Risk, and 13 at Lower Risk. Two counties have been given a two-week caution. A complete list of counties and their associated risk levels is available here.
